The U.S. healthcare system is the world’s largest and most expensive—estimated to have cost over $4 trillion in 2020—yet health outcomes are worse than in other advanced economies. Costs are so out of control that medical bills contribute to around 66% of all personal bankruptcies in the United States. It doesn’t have to be this way.
According to a report published in the Journal of the American Medical Association in 2019, nearly 25% of healthcare spending in the U.S. is wasted because of a system plagued by misaligned incentives, lack of coordination, and administrative complexities.
Health insurers substantially influence the healthcare ecosystem because they disburse 75 cents of every healthcare dollar. Despite decades of effort, incumbent insurers have made little progress in reigning in healthcare costs or incentivizing key stakeholders to produce better outcomes. According to the Harris Poll, U.S. consumers give health insurers the lowest rating of any sector of the healthcare system when it comes to making a positive difference.
Instead, for far too many consumers, health insurance adds a layer of complexity to an already complex system. According to another survey, fewer than 4% of Americans could accurately define the four basic health insurance terms: Deductible, Co-Insurance, Co-Pay, and Out-of-Pocket Maximum.
Oscar Health was founded to solve these problems and to provide consumers with access to the affordable, high-quality health care they deserve. Oscar Health recognized that doing so would require reorienting how customers see their health insurer and what they expect from it. To understand how we decided to analyze the business model of Oscar Health insurance and how does it work.
What is Oscar Health? How does Oscar Health insurance work?
Oscar Health, founded in 2012, is the first health insurance company built around a full-stack technology platform and a relentless focus on serving members. Oscar has created a suite of services by leveraging personalized data and helping members find quality care they can afford.
As of Jan ’22, Oscar had over a million customers. They include families seeking coverage that works for toddlers and their busy parents, adults with chronic conditions who know their care providers by their first names, and seniors choosing a benefits package that will serve them throughout their retirement years.
Too often, customers view legacy insurers as entities that merely take in monthly premiums and then pay medical claims. Oscar Health has built an insurance business model to serve as their guide to a confusing and fragmented system, helping them save money by optimizing their spending.
Full Stack Technology Platform: To guide members to the right care at the right time and value, Oscar has built a technology platform that provides an intuitive, seamless customer experience, leveraging the power of personalized data.
Oscar believes that real change in healthcare can only come from using personalized data to drive real-time actionable insights and recommendations. Oscar claims that nearly half of the first-time visits to primary care providers, or PCPs, by its members are recommended by Oscar’s platform.
Member Engagement Engine: Oscar has developed an intuitive consumer experience enabling members to take control of their healthcare decisions. That experience begins with trust and engagement, which it earns by providing members with features that help them navigate the many disconnected elements of the healthcare ecosystem.
Trust, engagement, and personalized data allow Oscar to help route members to the providers that can give them the right care, including virtual care, at the right time and cost.
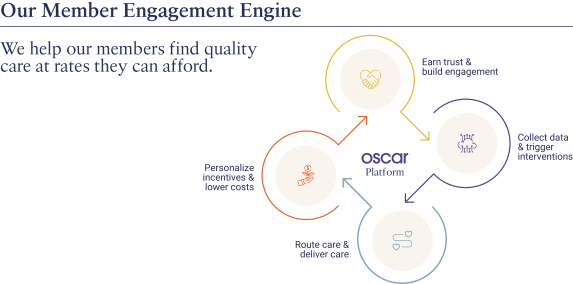
Oscar’s full-stack technology platform also permits it to offer personalized insights and benefits. The combination of all these factors—trust, engagement, care routing, and personalized insights—allows it to help its members find quality care at affordable rates. Oscar refers to this virtuous cycle as its member engagement engine.
Reinsurance: Oscar enters into reinsurance agreements to manage its exposure to unexpected fluctuations in MLR (medical loss ratio) and reduce its capital requirements. The Company enters into two arrangements: quota share reinsurance contracts and excess of loss (“XOL”) reinsurance contracts.
In quota share reinsurance, the reinsurer agrees to assume a specified percentage of the ceding Company’s losses arising out of a defined class of business in exchange for a corresponding percentage of premiums (in some cases, net of a ceding commission). In XOL reinsurance, the reinsurer agrees to assume all or a portion of the ceding Company’s losses in excess of a specified amount.
Under XOL reinsurance, the premium payable to the reinsurer is negotiated by the parties based on losses on an individual member in a given calendar year and their assessment of the amount of risk being ceded to the reinsurer because the reinsurer does not share proportionately in the ceding Company’s losses.
Lemonade Business Model: To Become the most loved insurance company
How does Oscar work for the members?
- Oscar members provide their symptoms data or health concerns using a computer or the smartphone app. This allows Oscar to intervene in real time.
- Members are then paired with their Care Team of five dedicated Care Guides and a registered nurse known as a Case Manager, supported by a regional team of licensed nurses and social workers. A member’s Care Team can answer questions about benefits, upcoming care, prescriptions, and much more and help them find high-quality providers.
- When the platform detects members seeking information about emergency care, Oscar puts them in immediate touch with doctors on its virtual platform.
- If required, Oscar’s ranking algorithm then uses artificial intelligence to match members to the best doctors for them. This technology saves both Oscar and the members money.
Oscar plans are named after metal tiers (Bronze, Silver, Gold, Platinum) to make it easy to compare options.
Secure
- Only for healthy people under 30 who want emergency coverage. Also called a catastrophic plan.
- Lowest premium, highest deductible.
Bronze
- A great option for healthy people who don’t see the doctor often and only take generic prescriptions.
- Low premium, a high deductible.
- Oscar pays 60% of covered health costs, and the member pays 40%.
Silver
- A great option for generally healthy people who expect to get routine care throughout the year and have generic drug prescriptions.
- Moderate premium, moderate deductible.
- Oscar pays 70% of covered health costs, and the member pays 30%.
Gold
- The best option for people who manage a chronic health condition, take brand-name drugs or have an upcoming procedure.
- Higher premium, lower deductible.
- Oscar pays 80% of covered health costs, and the member pays 20%.
Platinum
- Best for people managing a chronic health condition, taking multiple brand-name medications, or planning for a major procedure.
- Highest premium, lowest deductible.
- Oscar pays 80% of covered health costs, and the member pays 20%.
Business Model of Oscar Health Insurance
Oscar Health insurance business model is built around its member engagement engine and full stack technology platform, which drive high engagement and trust among members, collect and integrate data to produce real-time personalized insights, and help members find high-quality care options.
How does GoodRx work & make money | Business Model
Oscar’s revenue primarily consists of premiums from its members, which it receives as a fixed amount of PMPM. Oscar serves in three insurance markets- Individual, Small Group, and Medicare Advantage. Other revenue consists primarily of investment income.
Individual and Small Group: The Individual market primarily consists of policies purchased by individuals and families through Health Insurance Marketplaces. The Small Group market consists of employees of companies with up to 50 full-time workers in most states and up to 100 full-time workers in selected states.
Medicare Advantage: Oscar offers Medicare Advantage plans to adults age 65 and older who are eligible for traditional Medicare but select coverage through a private market plan instead.
Oscar Health generated $1.84 billion in 2021. Let’s see how Oscar calculates its annual revenue.
| Revenue (in $ Mn) | 2021 | 2020 | 2019 |
| Premiums before ceded reinsurance (1) | 2,713 | 1,672 | 1,041 |
| Reinsurance premiums ceded (2) | -882 | -1,217 | -572 |
| Premiums earned (1-2) | 1,831 | 455 | 469 |
| Investment income and other revenue | 8 | 8 | 19 |
| Total revenue | 1,839 | 463 | 488 |
Premiums Before Ceded Reinsurance: Premiums before ceded reinsurance primarily consist of premiums received from members or from CMS as part of the APTC program.
Reinsurance Premiums Ceded: Reinsurance premiums ceded represent the amount of premiums written that are ceded to reinsurers either through quota share or XOL reinsurance.
Investment Income and Other Revenue: Investment income and other revenue primarily includes interest earned and gains on the investment portfolio, along with income earned from administrative services performed as part of the +Oscar platform
















